When sleep does not come despite deep fatigue, it is natural to focus on the next strategy, supplement, or app. But in chronic insomnia, the sleep–wake system often gets caught in a loop of hyperarousal and conditioned wakefulness that keeps nights fragmented even when you are exhausted. Major guidelines recommend Cognitive Behavioural Therapy for Insomnia (CBT‑I) as first‑line care for adults because it systematically targets this loop and helps restore consolidated sleep. Canadian data indicate that insomnia symptoms are common and many adults report using sleep aids, highlighting the importance of accessible, evidence‑based behavioural options for people in Calgary and across the country (sources 8, 9).
This article explains, using high‑quality evidence, what keeps insomnia going, how CBT‑I works, and what adults can expect from therapy. We also outline everyday signs that the cycle is self‑maintaining, offer a Canada‑relevant context for seeking help, and provide a bounded ShiftGrit perspective on how beliefs and predictions may interact with the insomnia loop. Research findings and the ShiftGrit lens are kept clearly separate throughout.
- Guidelines recommend multi‑component CBT‑I as first‑line therapy for chronic insomnia in adults; sleep hygiene education alone is not recommended as a stand‑alone treatment (sources 1, 3).
- CBT‑I reliably improves difficulty falling asleep, night‑time awakenings, and sleep efficiency; gains in total sleep time can occur but may be gradual, particularly early in therapy (sources 2, 5, 6).
- Insomnia often persists through hyperarousal, conditioned wakefulness in the sleep environment, and sleep‑related worry that drive compensatory behaviours like napping and irregular schedules (sources 1, 7).
- Effective CBT‑I can be delivered in different formats (e.g., individual or group), with component evidence highlighting sleep restriction and stimulus control as key elements (sources 1, 4).
- From a ShiftGrit lens (conceptual), identity‑level beliefs may shape predictions and sleep effort; this lens is an explanatory scaffold and not a substitute for the evidence base.
How the insomnia pattern shows up day‑to‑day in adults
Chronic insomnia rarely looks like a single bad night. It tends to repeat as a set of cues, worries, and compensations that keep the system in a high‑arousal, low‑efficiency mode. The features below are common in lived experience and align with mechanisms discussed later; not everyone will have all of them.
- Lying awake in bed for long stretches, clock‑watching at 2–3 a.m., feeling “wired but tired” despite physical fatigue.
- Irregular schedules after poor nights (earlier bedtimes or sleeping in) and daytime naps that bring short‑term relief but reduce night‑time sleep pressure.
- Pre‑sleep loops of planning and “what if I can’t sleep?” that heighten mental and physical arousal.
- Using the bed for wakeful activities (phones, TV, email), which strengthens the bed–wakefulness link.
- Rising reliance on sleep aids or alcohol to “knock out,” often with diminishing returns and grogginess the next day.
Downstream, adults often notice concentration dips at work, irritability, and reduced motivation for evening plans or exercise. After a rough night, protective steps like napping or extending time in bed may feel sensible; over time, these can erode homeostatic sleep drive and circadian anchors, increasing the likelihood of another fragmented night. Recognizing this escalation pattern is a first step toward targeted change.
CBT‑I as first‑line care for adult chronic insomnia: what changes and why it matters
Across major adult guidelines, multi‑component CBT‑I is recommended as the initial treatment for chronic insomnia, while sleep hygiene education alone is not advised as a stand‑alone therapy (sources 1, 3). This standard‑of‑care positioning reflects consistent evidence that structured behavioural and cognitive components directly target the processes that keep insomnia going.
Meta‑analytic syntheses show that CBT‑I improves core outcomes: people tend to fall asleep faster, spend less time awake during the night, and achieve higher sleep efficiency (sources 2, 5). These changes reflect better consolidation of sleep rather than simply “more time in bed.” Effects on total sleep time can also occur, but they vary across trials and individuals (sources 2, 6). Early in treatment, some adults experience temporary limits on time in bed due to sleep restriction therapy; as efficiency improves, the sleep window can be expanded and sleep duration commonly follows.
Therapist‑delivered, multi‑component CBT‑I is well supported. Evidence also indicates that specific single components—particularly sleep restriction and stimulus control—carry substantial effects, and that CBT‑I can be delivered in different formats (e.g., individual or group) to accommodate access and preferences (sources 1, 4). Variation in components and delivery may contribute to heterogeneity in outcomes, reinforcing the value of tailoring to an individual’s maintaining factors.
Guidelines emphasise shared decision‑making. When CBT‑I is not accessible or if response is incomplete, additional steps may be considered through a collaborative risk–benefit discussion (source 3). Overall, the evidence base supports CBT‑I as a robust, first‑line option for adult chronic insomnia, with benefits that generalize across the central problems of initiation and maintenance of sleep (sources 1, 2, 5).
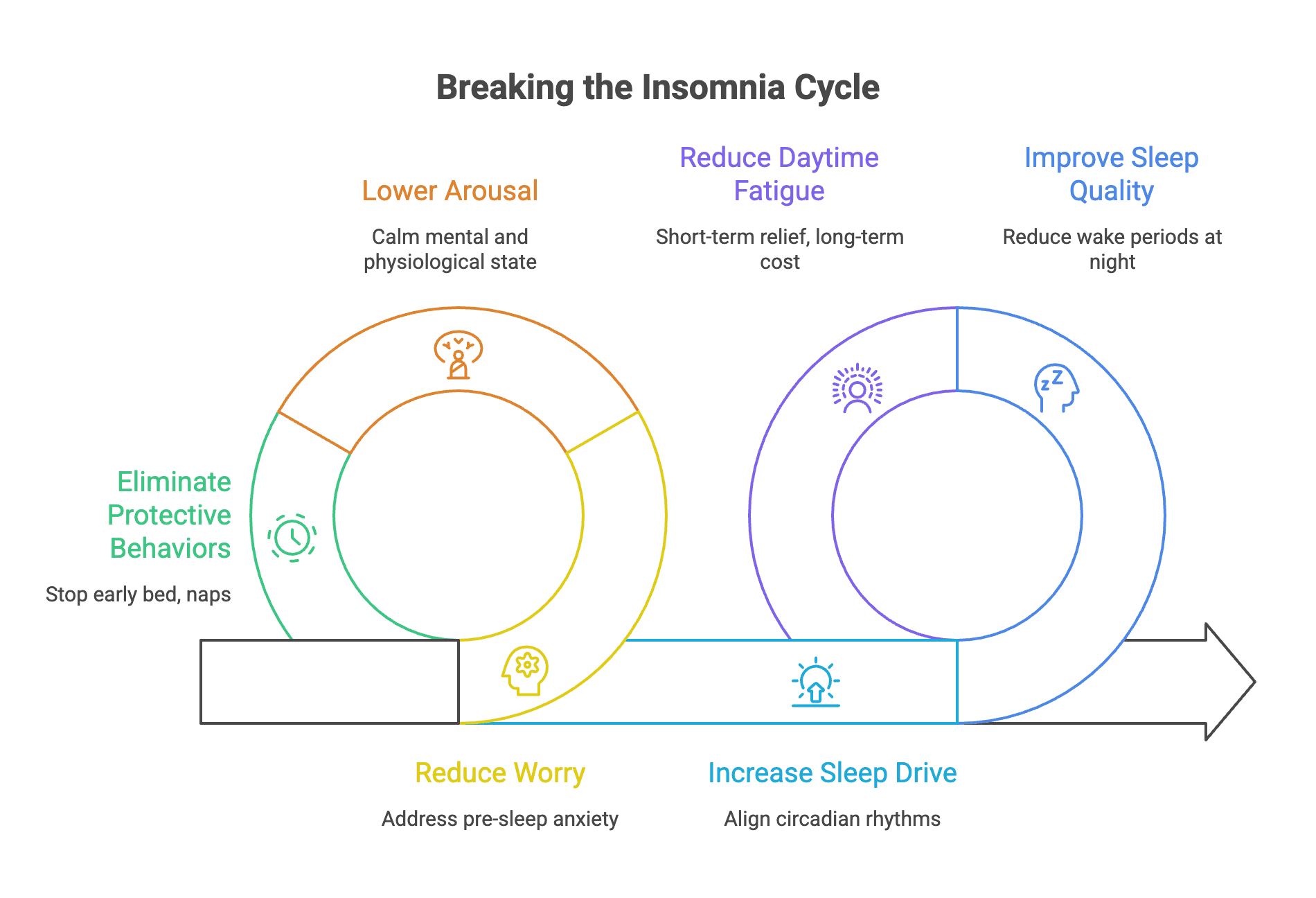

What keeps insomnia stuck: hyperarousal, conditioned wakefulness, and sleep‑related anxiety
A leading account of chronic insomnia highlights hyperarousal—heightened cognitive, emotional, and physiological activation that persists into the night (source 7). When mental rehearsal, worry, and physiological tension remain elevated, the brain struggles to make the transition from wake to sleep. This is more than “stress”; it is a 24‑hour tendency toward activation that can undermine both sleep onset and continuity.
Conditioned arousal further links the bed and bedroom with wakefulness: spending extended periods awake in bed, using the bed for wakeful activities, or “trying hard” to sleep trains the nervous system to associate the sleep environment with alertness (sources 1, 2, 7). Stimulus control—a core CBT‑I component—exists to reverse this learning by reducing wakeful time in bed and re‑associating the bed with sleepiness.
Compensatory or “safety” behaviours often feel protective yet can perpetuate insomnia. Extending time in bed after a poor night, sleeping in, irregular bedtimes, or daytime napping may reduce homeostatic sleep drive and destabilize circadian timing, setting the stage for lighter, more fragmented sleep (sources 1, 7). This is why CBT‑I includes schedule regularity and carefully titrated time in bed: to rebuild sleep pressure and re‑establish predictable timing signals.
Sleep‑related worry and misappraisal also contribute. Catastrophic predictions (“Tomorrow will be ruined”), clock‑monitoring, and scanning for sleep cues amplify arousal and heighten attention to sleep‑disrupting sensations (source 7). Cognitive strategies in CBT‑I address these patterns by testing predictions and reducing control‑based behaviours that backfire.
These processes commonly interact in a self‑reinforcing loop: a poor night produces fatigue and worry; compensations follow (naps, early bedtime) that reduce sleep drive or shift timing; the bed becomes a cue for wakefulness; another poor night confirms the threat prediction (sources 1, 7). Importantly, insomnia mechanisms are heterogeneous—physiology and behaviour vary by person—so effective therapy targets the specific maintaining factors identified in assessment (sources 2, 7).
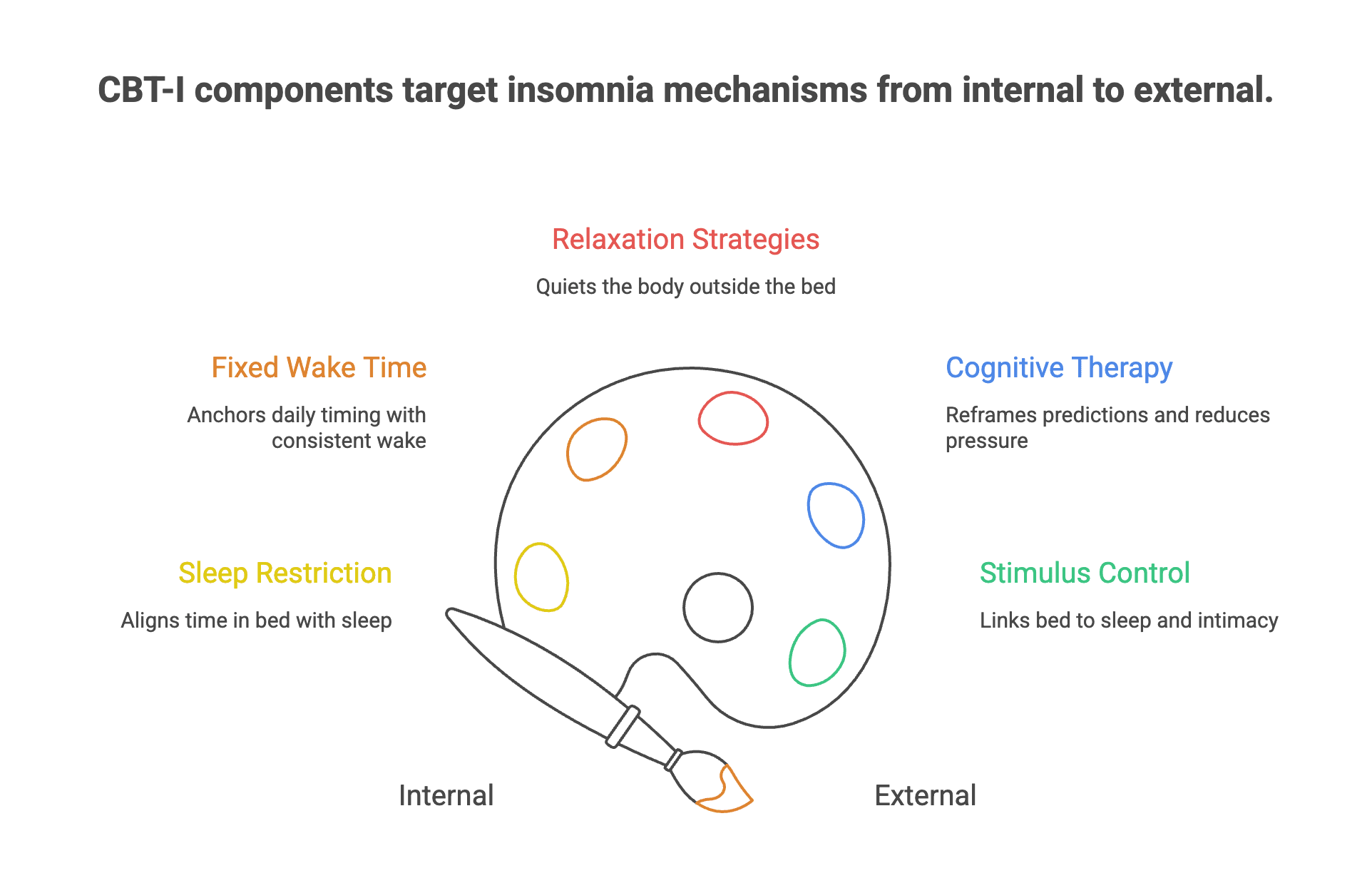

Components and delivery: how adults access effective CBT‑I and why format fit matters
Structured CBT‑I packages consistently perform well in trials, and component‑level analyses indicate that sleep restriction and stimulus control are key active elements within effective protocols (sources 2, 4). These behavioural levers rebuild sleep pressure and re‑link the bed with sleep, while cognitive strategies address misappraisal and sleep‑related worry.
Delivery formats can be adapted. Evidence supports therapist‑delivered CBT‑I in individual and group settings, with variable dose and length to fit clinical realities (sources 1, 4). This flexibility matters for access, preferences, and tolerability—especially when starting with behavioural changes like a fixed wake time or temporary sleep window compression.
Guidelines recommend starting with CBT‑I and then engaging in shared decision‑making about next steps if symptoms persist or if therapy access is limited (sources 1, 3). In Canada, insomnia symptoms are common and many adults report using sleep aids, underscoring the need for accessible behavioural options that address maintaining mechanisms rather than only providing short‑term sedation (sources 8, 9). Response varies by individual, which supports an approach that emphasises the most relevant components for the person’s presentation and goals (sources 2, 4).
CBT‑I components for adults: targets, typical practices, and evidence notes
| Component | Mechanism target | Typical practices | Evidence notes |
|---|---|---|---|
| Sleep restriction | Low sleep drive; fragmented consolidation | Initial sleep window near actual sleep time; fixed wake time; gradual expansion as efficiency improves | Identified as a key active element in component analyses; central in multi‑component CBT‑I |
| Stimulus control | Conditioned wakefulness in bed/bedroom | Bed only for sleep; go to bed when sleepy; leave bed when awake; consistent wake time | Core behavioural element with strong support; reconditions bed–sleep association |
| Cognitive therapy | Sleep‑related misappraisal and worry | Test catastrophic predictions; reduce clock‑checking; shift attention from sleep control | Supported within multi‑component CBT‑I; targets pre‑sleep cognitive arousal |
| Relaxation training | Physiological arousal | Brief wind‑down; breathing or muscle relaxation | Supportive adjunct within CBT‑I; not typically sufficient alone |
| Sleep hygiene education | Non‑specific sleep‑related habits | General advice (caffeine, light, exercise, environment) | Not recommended as stand‑alone therapy; best as adjunct to core components |
Claim boundary: Summarises supported components and their typical use; does not prescribe a one-size-fits-all protocol or rank components beyond sources.
How CBT‑I targets the insomnia mechanisms
CBT‑I is designed to change the drivers that keep insomnia going. Behavioural components compress and then expand time in bed to rebuild homeostatic sleep drive, hold a consistent wake time to stabilise circadian cues, and minimise time awake in bed to re‑associate the bed with sleep. Cognitive strategies reduce sleep‑related misappraisal and the tendency to monitor and control sleep in ways that raise arousal (sources 1, 2).
In practice, this often means: 1) setting an initial sleep window close to actual sleep time and protecting a fixed wake time, 2) going to bed when sleepy and leaving the bed if awake to prevent conditioning the bed as a wake cue, 3) testing catastrophic predictions about next‑day function and scaling back clock‑checking, and 4) using a brief wind‑down to lower pre‑sleep physiological tension. Research supports multi‑component packages and highlights sleep restriction and stimulus control as central behavioural levers (sources 1, 2, 4). Effects on total sleep time may emerge alongside improved efficiency and consolidation rather than immediately (source 6).
Insomnia in Canada: why access and fit matter
Canadian reports indicate that insomnia symptoms are common among adults and that many people use sleep aids to cope (source 8). Longitudinal analyses also describe trends in night‑time insomnia symptoms over time (source 9). For adults in Calgary, this context underscores why a therapy‑first approach that targets maintaining mechanisms is emphasized in guidelines and why practical delivery options—such as group formats or variable dosing—can help more people engage with CBT‑I (sources 1, 3, 4).
Because chronic insomnia is maintained by interacting behavioural and cognitive processes, change tends to be cumulative. Early improvements often show up as fewer long wake periods and more predictable timing; duration gains may follow as the sleep window expands. Shared decision‑making about format, pacing, and next steps can help therapy fit real‑life constraints while keeping the focus on evidence‑based targets (sources 1, 3).
From a ShiftGrit lens: how beliefs and predictions can nudge the loop (conceptual)
Research identifies mechanisms that CBT‑I targets—hyperarousal, conditioned wakefulness, and sleep‑related misappraisal (sources 1, 2, 7). From a ShiftGrit conceptual perspective, identity‑level beliefs may influence how adults interpret a poor night and how much “sleep effort” they deploy. For example, “I Am Not In Control” can fuel micromanagement (rigid rituals, clock‑watching) that elevates arousal; “Bad Things Are Going To Happen” can drive catastrophic predictions about the next day; and “I Am Defective” can turn a variable night into self‑blame and withdrawal. This mapping is an explanatory scaffold, not a proof of mechanism or a replacement for CBT‑I.
Within this conceptual frame, behaviour‑first changes create disconfirming experiences: limit time in bed to rebuild sleep pressure, leave bed when awake to retrain the bed–sleep association, hold a fixed wake time to stabilise cues, and run small experiments that test catastrophic predictions. These ideas align with CBT‑I principles without claiming additional efficacy. Individual loops differ; the aim is to notice the predictions and protective behaviours that keep your loop active and to adjust them safely and systematically.
Identity-Level Therapy for Insomnia
From a ShiftGrit lens, insomnia may persist when beliefs about control, safety, and next-day consequences amplify sleep-related threat and drive protective behaviours. Those behaviours can offer short-term relief while inadvertently maintaining arousal, conditioned wakefulness, and anticipatory worry. In this interpretation, treatment focuses on disrupting the loop between belief, prediction, behaviour, and reinforcement rather than only reacting to the surface symptom of poor sleep.
It’s organized around three pillars:


ShiftGrit Core Method™
Our structured framework for breaking outdated identity patterns.
Learn more

The Pattern Library
Real-world examples of loops like perfectionism, procrastination, and shutdown.
Learn more

The Glossary
Clear definitions that keep the language sharp and the process transparent.
Learn moreLimiting Beliefs Commonly Linked with Insomnia Therapy
These identity-level patterns frequently show up for clients seeking insomnia therapy. Explore the beliefs to learn the “why” and how therapy can help you recondition them.


“I Am Not in Control”
When “I Am Not In Control” is running the show, everything feels like too much. You either grip harder—rigid routines, hypervigilance—or give up entirely. Underneath it all is…
Explore this belief

“Bad Things Are Going To Happen”
Always on edge. Always preparing for the worst. This belief doesn’t keep you safe — it keeps you stuck. But it can be rewired.
Explore this belief

“I Am Defective”
“I Am Defective” is a deep-rooted core belief that can leave a person constantly scanning for signs that they’re flawed, broken, or fundamentally unworthy of love and acceptance.…
Explore this beliefWant to see how these fit into the bigger pattern map? Explore our full Limiting Belief Library to browse all core beliefs by schema domain and Lifetrap.
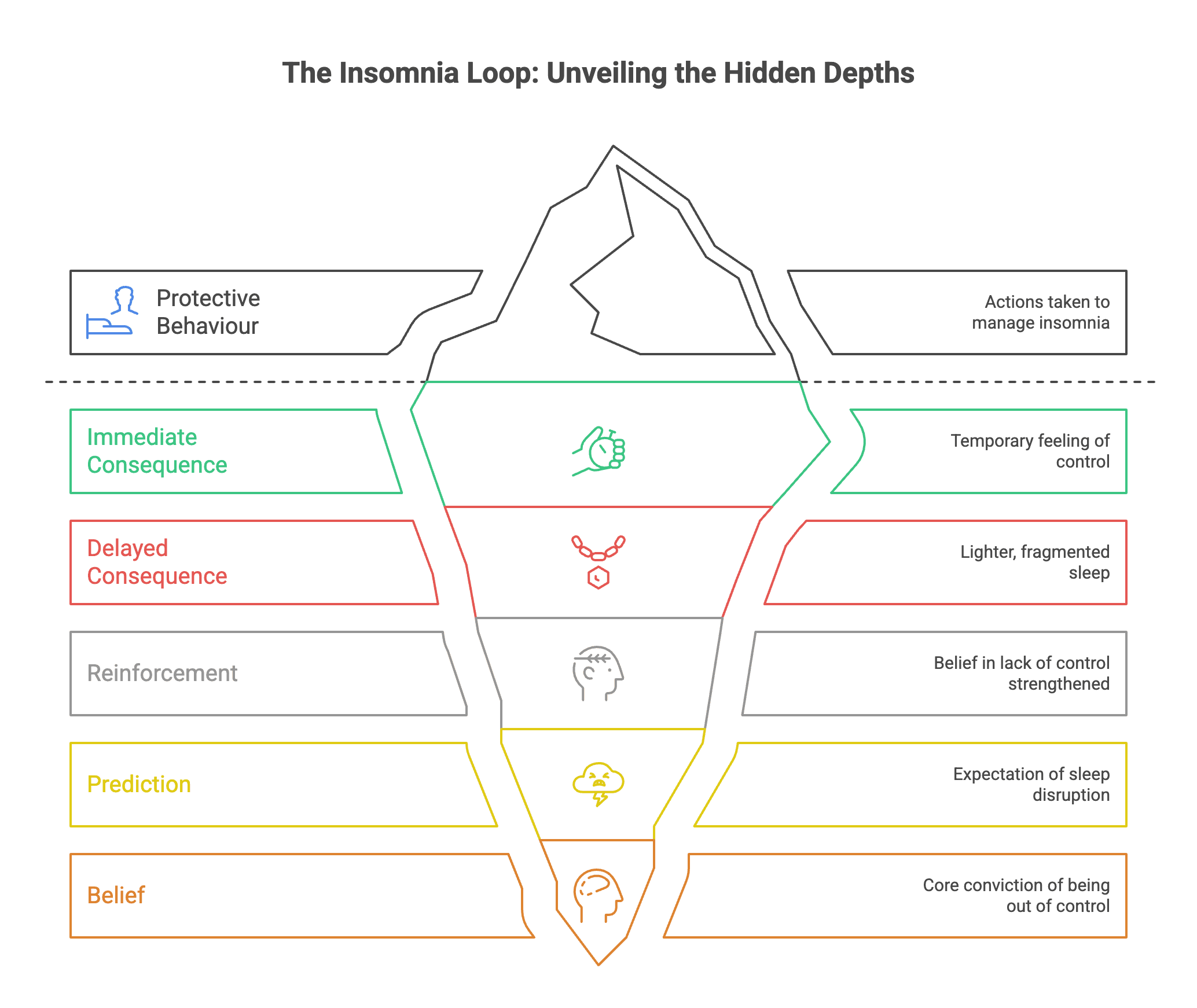
Identity‑Level Therapy (ILT): a bounded framing for insomnia‑maintaining loops
ILT considers how identity‑level beliefs can bias interpretations and protective behaviours around sleep. A common loop is: Trigger (bedtime or a recent poor night) → Prediction (“If I don’t sleep 8 hours, I will fail tomorrow”) → Arousal spike (monitoring, worry, muscle tension) → Protective behaviours (early bed, sleeping in, naps, clock‑checking) → Short‑term relief but reduced sleep drive or conditioned wakefulness → Night‑time wakefulness → Perceived confirmation of the prediction. Therapy aims to alter the predictions and behaviours that maintain the loop.
In this frame, behaviour‑first shifts are central: consolidate time in bed and protect a fixed wake time; retrain the bed–sleep link by leaving bed when awake; reduce control‑based behaviours that backfire (for example, limit clock‑checking and schedule worry earlier); and test catastrophic predictions with small, safe experiments. This is a clinical framing that complements, but does not replace, the guideline‑supported CBT‑I approach. It does not imply a guaranteed outcome or a specific timeline.

Bringing it together
Chronic insomnia persists when worry, arousal, and compensations teach the brain that the bed is a place to be awake. CBT‑I directly targets this loop: it rebuilds sleep pressure, re‑links the bed with sleep, and helps recalibrate sleep‑related predictions. Evidence supports CBT‑I as first‑line care for adults, with flexible delivery options and component insights that allow for tailoring (sources 1, 2, 4).
For adults in Calgary, the practical path usually starts with a structured behavioural plan, careful monitoring, and shared decision‑making. Early changes may look like fewer long wake periods and a steadier schedule; duration often follows as consolidation improves. If access is limited or response is partial, options can be adapted collaboratively in line with guidelines. Whatever the starting point, keeping focus on the maintaining processes—rather than chasing a perfect sleep—helps the cycle unstick.
Frequently asked questions
What is CBT‑I and how does it work for chronic insomnia?
Cognitive Behavioural Therapy for Insomnia (CBT‑I) is a structured, multi‑component therapy recommended as first‑line care for adults with chronic insomnia. It rebuilds sleep pressure, re‑associates the bed with sleep, stabilises timing, and reduces sleep‑related worry. Guidelines and meta‑analyses show improvements in falling asleep, fewer night awakenings, and higher sleep efficiency. Components like sleep restriction and stimulus control are key behavioural levers supported by evidence.
How quickly should I expect results from insomnia therapy?
Timelines vary, but early gains often appear as fewer long wake periods and a steadier schedule. Because sleep restriction initially limits time in bed to rebuild sleep pressure, total sleep time may not rise immediately. As efficiency improves, the sleep window is usually expanded and duration can follow. Meta‑analytic work indicates sleep duration can improve, though effects differ by study and person.
Can sleep hygiene alone fix chronic insomnia?
Sleep hygiene education can support good routines but is not recommended as a stand‑alone treatment for chronic insomnia. Major guidelines advise multi‑component CBT‑I as the initial approach because it directly targets the mechanisms that maintain insomnia. Effective elements include sleep restriction, stimulus control, and cognitive strategies. Hygiene advice is best used as an adjunct to these core components.
Do I need medication for insomnia, or can therapy be enough?
Guidelines recommend starting with CBT‑I for chronic insomnia in adults. Many people improve with behavioural and cognitive strategies that consolidate sleep and reduce arousal. If access is limited or response is incomplete, next steps can be considered through shared decision‑making. Decisions about medication are individualised and typically follow an informed discussion of risks and benefits.
What delivery formats are available for CBT‑I in Calgary?
Research supports CBT‑I delivered by therapists in individual or group formats, with variable dose and length to fit practical needs. Component evidence highlights sleep restriction and stimulus control across formats. In Calgary, availability depends on local services, but the evidence base supports choosing a format that you can access and engage with. Shared decision‑making helps match format and pacing to your goals.
Sources for the article
Jack D. Edinger; J. Todd Arnedt; Suzanne M. Bertisch; Colleen E. Carney; John J. Harrington; Kenneth L. Lichstein; Michael J. Sateia; Wendy M. Troxel; Eric S. Zhou; Uzma Kazmi; Jonathan L. Heald; Jennifer L. Martin. Behavioral and psychological treatments for chronic insomnia disorder in adults: an American Academy of Sleep Medicine clinical practice guideline. Journal of Clinical Sleep Medicine. 2021.
Jack D. Edinger; J. Todd Arnedt; Suzanne M. Bertisch; Colleen E. Carney; John J. Harrington; Kenneth L. Lichstein; Michael J. Sateia; Wendy M. Troxel; Eric S. Zhou; Uzma Kazmi; Jonathan L. Heald; Jennifer L. Martin. Behavioral and psychological treatments for chronic insomnia disorder in adults: systematic review, meta-analysis, and GRADE assessment. Journal of Clinical Sleep Medicine. 2021.
Amir Qaseem; Devan Kansagara; Mary Ann Forciea; Molly Cooke; Thomas D. Denberg. Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Annals of Internal Medicine. 2016.
James M. Trauer; Mary Y. Qian; Joseph S. Doyle; Shantha M. W. Rajaratnam; David Cunnington. Cognitive Behavioral Therapy for Chronic Insomnia: A Systematic Review and Meta-analysis. Annals of Internal Medicine. 2015.
The neurobiology, investigation, and treatment of chronic insomnia
Prevalence of insomnia and use of sleep aids among adults in Canada
Trends in nighttime insomnia symptoms in Canada from 2007 to 2021